Community Diagnostic Centres (CDC): Workforce Insights
What is the national CDC Programme all about?
The national Community Diagnostic Centres (CDC) programme was borne from Professor Sir Mike Richards’ national review of diagnostics (2020), and highlights “the need for radical investment and reform of diagnostic services”. One key recommendation from the report was to rapidly establish Community Diagnostic Centres (CDCs) to provide diagnostic services for cancer, cardiac, respiratory and other conditions. From the launch of the programme in May 2021, to January 2022, the national CDC programme delivered more than 360,000 additional diagnostic tests.
How did Attain support the CDC programme?
Attain have considerable experience in developing workforce solutions and improving diagnostic services across the NHS. As part of the National CDC programme, Attain are supporting multiple Integrated Care Systems (ICS) to increase diagnostic capacity and speed up elective recovery. The first system to launch CDCs with Attain’s embedded support, the Cheshire and Merseyside ICS, stood up five CDC sites within six months of launching their programme.
The rapid development and roll-out of the CDC programme has not been without challenge, including requirements for system-wide leadership and governance, collaborative working across organisational boundaries, digital interoperability, and a need to support an already stretched diagnostic workforce.
How did we approach system-wide workforce challenges?
The Richards’ Report provides insight into long-standing workforce challenges; for example, it is estimated that an additional 2,000 Radiologists and 4,000 Radiographers are required to meet rising demand over the next five years. With the NHS workforce already stretched, adding additional capacity through the CDC programme requires a focus on supporting the diagnostic workforce and developing realistic short, medium and long-term workforce solutions.
At the start of each system’s CDC programme, Workforce Steering Groups were set up to bring together representatives from Diagnostic Networks, Providers, the ICS, and arms-length bodies such as HEE. Before developing workforce implementation plans, a roadmap was agreed, based upon the Six Steps Approach to Integrated Workforce Planning:

Each system conducted a baseline data collection, in partnership with HEE, to assess the current size and composition of the diagnostic workforce. Once verified, and in combination with activity profiles from the CDC business case requirements, this data was used to model the size of each system’s diagnostic workforce gap. For one system, the estimated workforce gap is shown below:
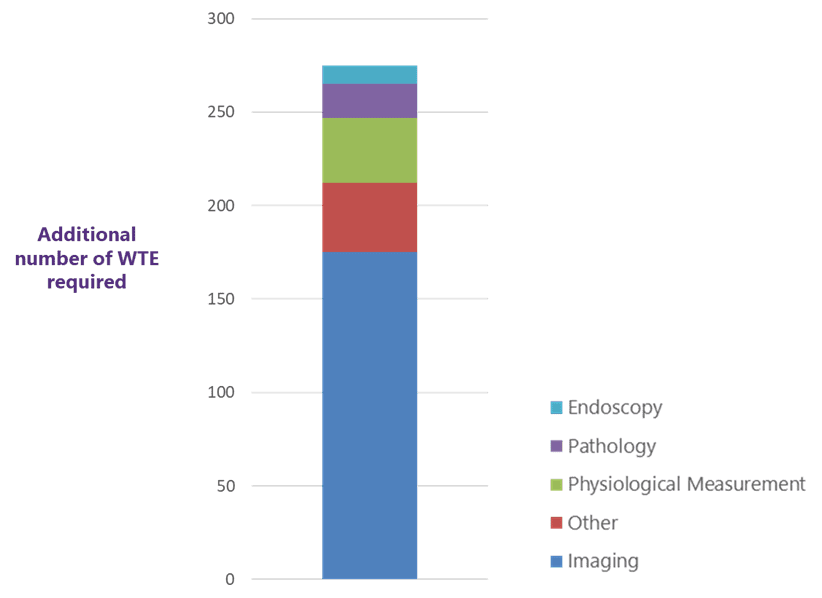
Qualitative intelligence was also gathered via meetings, workshops and surveys. The Workforce Steering Groups then used this combination of quantitative and qualitative information to identify key themes and areas of focus:

This bundle of solutions formed initial Workforce Delivery Plans. In the short-to-medium term, international recruitment, pay harmonisation, and digital staff passports were key areas of focus. Longer-term interventions, such as the development of Training Academies, increased apprenticeship placements, and systematic data-driven workforce planning were identified as key to the sustainable operation of the system’s CDCs.
What difference is the CDC programme making to people’s lives?
The Cheshire and Merseyside system alone has delivered more than 15,000 additional diagnostic tests across imaging, pathology, endoscopy and physiological measurement. This means that patients are being seen more quickly, diagnoses are faster, and timely treatment can commence.
To find out more about how Attain can help to support your CDC programme or wider diagnostic services please contact Struan Coad or Sophia Malik
More about our Cancer and Diagnostics expertise
Contact us to discuss your challenges
Get in touch with us to learn more about how we can support you in addressing your challenges.
Complete our simple form and we’ll call you right back, alternatively just email: