Five critical factors for a successful Acute Service Review
Reviewing acute services is not a new idea. Almost every trust has undertaken reviews at service or trust level as part of a cost reduction or transformation programme. Some have undoubtedly driven efficiencies, but it has become clear from our dealings with several systems that not all reviews deliver the desired efficiencies. Here we explore the critical success factors, based on our experience, of an acute service review.
System-wide acute reviews are more efficient
Whilst it is possible to improve quality and create efficiency savings at a single trust level, we believe the benefits at trust level may offer diminishing returns. Many trusts have now recognised that they cannot work in isolation and that the scale of transformation required to make services sustainable can only be achieved through partnership with neighbouring trusts.
System-wide acute reviews are being initiated across the NHS with the aim of achieving greater economies of scale and more sustainable models of care across a broader population. This does make the review more complex, and the cultural and political challenges remain, however:
System-wide Acute Service Reviews, done well, have the potential to drive a new level of clinical conversation that crosses organisational boundaries and identifies significant opportunities to improve quality and safety as well as deliver financial savings at system level.
Acute Service Review Framework
Attain have supported a number of system-wide and single trust acute service reviews using our Acute Service Review Framework shown below:
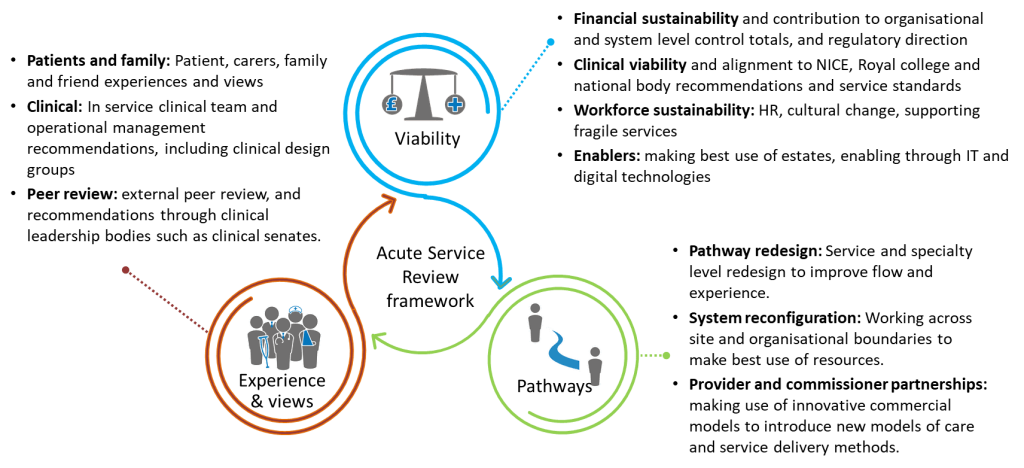
Five critical factors for a successful Acute Service Review:
Five key factors that are vital to successful and efficient implementation of an acute review:
Building trust through independent facilitation
Clarity on scope and breadth to maintain focus
Gaining momentum through dedicated programme management and analytics
Robust governance arrangements for timely decision making
Commercial acumen to develop vehicles for new models
1. Building trust through independent facilitation
Through independent facilitation, we aim to address the serious risks that are present when systems attempt to implement change alone:
- One trust can be accused of dominating others. In some systems there exist very traditional and even combative relationships between large teaching hospitals and neighbouring DGHs. The reality is that the critical mass required to achieve tertiary status is generated through neighbouring DGH populations and referral patterns. We have found that acting as an “honest broker” can help trusts to explore their mutual dependencies and build trust between the clinical teams.
- Lack of innovation. We use our network of clinical leaders across the country to present ‘clinical challenge’ that inspires local clinical teams to consider the “art of the possible”, highlighting examples that can be tailored for local use. This can shorten the process of identifying ideas and solutions and drive greater innovation than might be achieved through local peer-to-peer challenge.
- Commissioner concerns. We find commissioners value the level of independence that we bring – particularly where there are broken or challenged relationships within the system. The balance between provider vs commissioner-led transformation can be hard to achieve without a level of independence. Our acute service review teams have deep commissioner and provider expertise to ensure we can build trust on both sides.
2. Clarity on scope and breadth to maintain focus
It’s important to agree the scope and breadth of the review at the outset – and stick to it.
Scope creep is one of the most common reasons why projects and programmes overrun or do not achieve expected benefits.
The complexity of acute care, and interdependencies with primary, community and intermediate care means it’s tempting to expand the scope with every new conversation. Project meetings can go around in circles, risking low engagements, making consensus in the case for change or new clinical model much more difficult to build. We build in time during the “mobilisation” phase to agree an achievable scope within a proposed timescale and deliver benefits at the scale and pace needed.
If additional areas are identified throughout the review process, we capture any ideas or issues and recommend clients hold them for a secondary phase of review.
3. Gaining momentum through dedicated programme management and analytics
It sounds obvious, but we often find clients start a review process with no dedicated programme management or analytical support. This can be tough for the teams delivering the work on top of their “day job” and without a structured programme approach, which can result in lost momentum. Operational commitments regularly encroach on the time people intend to use for project and programme commitments.
Expert programme management, coupled with dedicated analytical expertise can ensure the pace and drive is maintained throughout the review process.
Attain’s Acute Service Review Framework, used by our experienced programme managers, help to shape a programme into four stages of delivery as shown below:
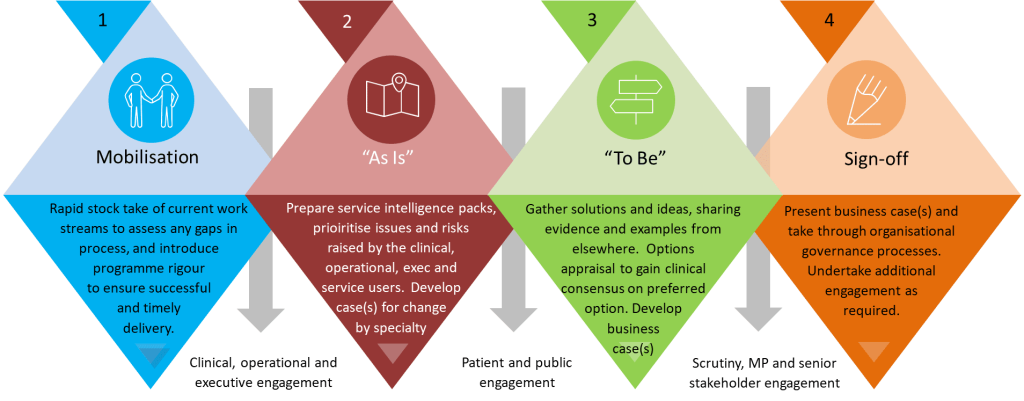
4. Robust governance arrangements for timely decision making
Programme governance is a whole topic in itself – but it’s critical to maintaining pace and momentum. Getting the balance right can be tricky, and there’s no doubt that a tailored approach is needed. We recommend a programme board/steering group for the major decisions including sign-off at each of the four stages, and then a regular operational group to manage the day-to-day delivery of the work.
Service specific groups should oversee the development of clinical models, along with patient/public engagement events to ensure appropriate engagement in the development of options.
5. Commercial acumen to develop vehicles for new models
This might not be your first thought when preparing a skills profile for an acute service review team. However, we have found the implementation of a new model of care can be hindered drastically if a suitable commercial model is not identified as part of the options appraisal. This is particularly relevant for system-level reviews that would like to implement innovative models of care across traditional organisational boundaries.
We always use the expert experience of our commercial team to ensure that as the clinical, operational and activity models are developed for the new models of care, we can also include a commercial / contractual options appraisal to identify the most appropriate commercial vehicle for implementation.
Contact us to discuss your challenges
Get in touch with us to learn more about how we can support you in addressing your challenges.
Complete our simple form and we’ll call you right back, alternatively just email: